The landscape of North American medical education is undergoing a fundamental shift. Traditionally reliant on static, classroom-bound instruction, high-stakes clinical certifications are now moving toward tech-first, hybrid models. This article analyzes the physiological and logistical advantages of blended learning in the healthcare sector, demonstrating how digital theory combined with intensive physical assessment produces more capable, ready-to-act medical professionals in high-pressure environments.
Contents
In the high-stakes world of emergency medicine, the margin for error is non-existent. For decades, the gold standard for clinical readiness was defined by long hours in a physical classroom, listening to lectures and watching instructional videos. However, the rapid acceleration of digital infrastructure has forced a re-evaluation of how we maintain the “clinical pulse” of our healthcare workforce.
Across North America, from major medical hubs in the United States to growing healthcare sectors in Alberta, the model for acquiring Basic Life Support (BLS) is evolving. We are moving away from the “all-day seminar” and toward a tech-first, blended learning architecture. This isn’t just a matter of convenience; it is a strategic improvement in how the human brain retains life-saving information.
The Cognitive Science of Spaced Learning
The traditional “massed learning” approach—where a student is bombarded with eight hours of information in a single day—is notoriously inefficient for long-term retention. In a clinical setting, where a nurse or doctor may not need to perform high-performance CPR for months at a time, the “forgetting curve” is a significant threat to patient outcomes.
Tech-first platforms utilize “spaced learning.” By allowing medical professionals to complete the theoretical and cognitive components of their certification online, they can digest complex algorithms at their own pace. Digital modules allow for interactive simulations, where a student must make split-second decisions on airway management or cardiac rhythms before they ever step foot in a lab. This builds a stronger cognitive foundation, ensuring that when they do arrive for their physical assessment, their mental “scripts” are already locked in.
High-Fidelity Feedback and the Physical Component
While the theory has moved to the cloud, the physical application of life-saving skills remains grounded in reality. You cannot learn the exact resistance of a human sternum through a screen.
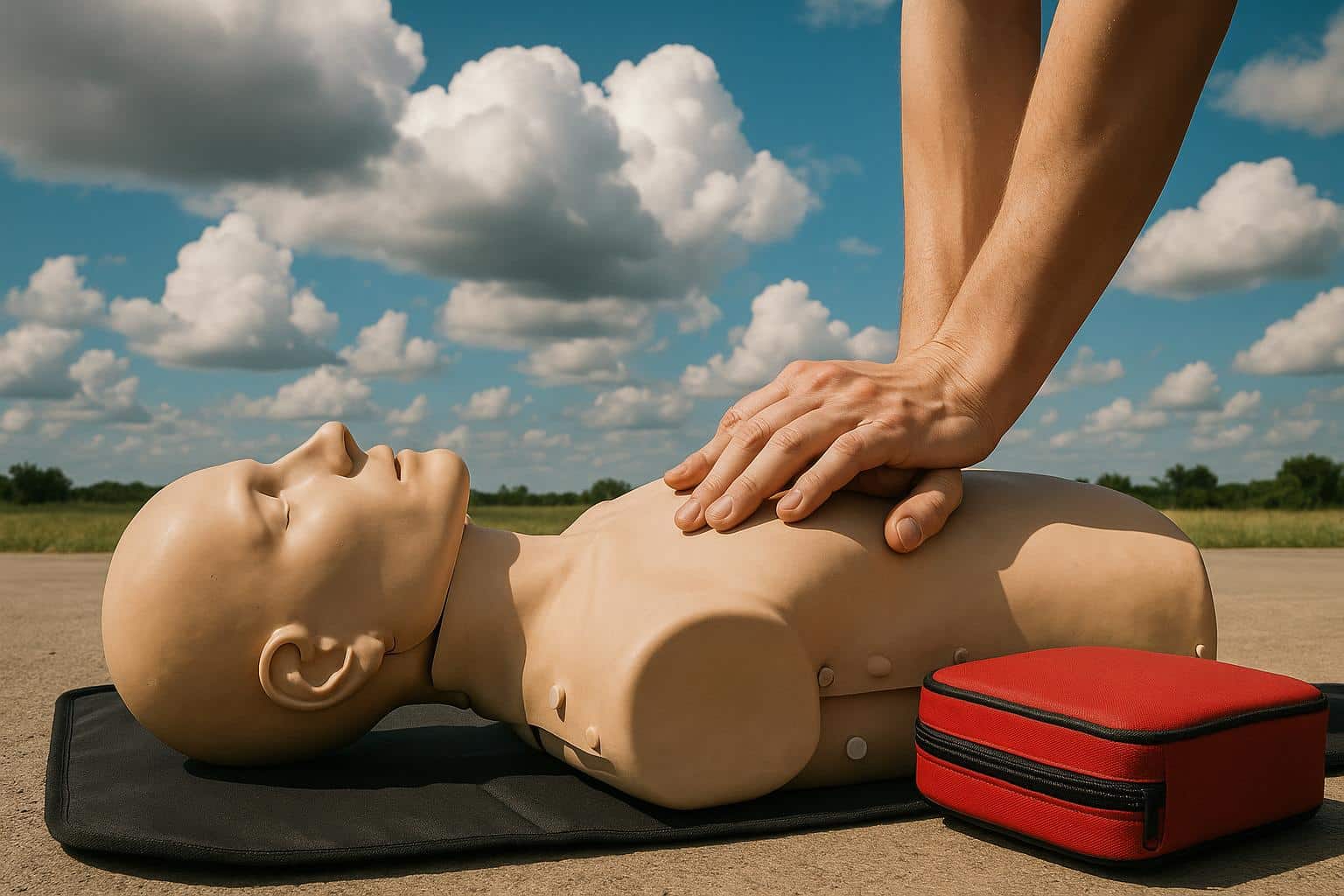
The “Blended” portion of modern training involves high-intensity, in-person skills sessions. Today’s training facilities use high-fidelity mannequins equipped with digital sensors. These sensors provide real-time data on:
- Compression Depth: Ensuring the heart is being physically compressed enough to circulate blood.
- Recoil: Verifying the chest fully expands to allow the heart to refill.
- Rate: Maintaining the 100–120 beats per minute required for optimal perfusion.
This tech-integrated feedback loop turns a subjective practice session into an objective data-driven assessment. It ensures that every professional who leaves the facility is capable of maintaining a patient’s viability until advanced life support can be established.
Logistical Resilience in Healthcare Systems
The logistical strain on modern healthcare systems is at an all-time high. Pulling a full team of paramedics or emergency room nurses off the floor for a two-day training retreat creates dangerous gaps in community coverage.
By utilizing tech-first providers like Coast2Coast First Aid & Aquatics (https://www.c2cfirstaidaquatics.com/), healthcare administrators can implement “just-in-time” training. Staff can complete their online theory during low-volume shifts or from home, attending only a brief, 2-to-3-hour physical check-off. This maximizes “uptime” for the medical facility while ensuring every staff member meets the rigorous national standards for resuscitation.
The future of clinical authority is digital-first but hands-on. By embracing the hybrid model, we are creating a more resilient, more capable, and more efficient healthcare front line.
FAQ: The New Standard of Clinical Training
1. Is a blended BLS certificate viewed differently by hospitals?No. Leading organizations like the Heart and Stroke Foundation and the American Heart Association have fully endorsed blended learning. The certificate issued is identical to the one earned in a traditional classroom, as the in-person skills assessment remains a mandatory requirement.
2. How does BLS differ from Standard First Aid?Standard First Aid is designed for the general public and workplace safety. Basic Life Support (BLS) is a higher-tier certification specifically for healthcare professionals (nurses, doctors, dental professionals). It focuses on high-performance team-based CPR, bag-valve-mask ventilation, and advanced clinical communication.
3. Can I complete the physical assessment virtually?No. To maintain clinical authority and legal compliance, a certified instructor must physically witness and grade your ability to perform compressions and ventilations on a mannequin. Virtual-only courses are generally not accepted in a medical environment.
4. How often should clinical teams recertify their BLS skills?While the standard certification period is typically one year for healthcare professionals, research suggests that physical skill degradation happens much faster. Many high-performance teams, such as those in trauma centers, perform quarterly “low-dose, high-frequency” training to stay sharp.5. Does tech-first training work for older medical professionals?Yes. Modern blended learning platforms are designed with high accessibility and intuitive user interfaces. The goal is to reduce administrative friction, not increase it, allowing professionals of all experience levels to focus on the life-saving science.